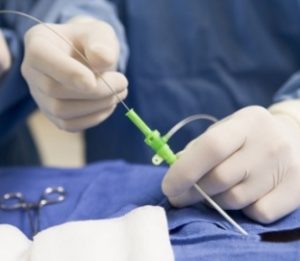
Principle of treating skin veins (varicose veins) with injections is the injection of a sclerosing agent (liquid or foam), which causes damage to the vessel wall, leading to inflammation and adhesion (closure). The inflammatory reaction results in thickening of the vessel wall, which transforms into a firm, indurated scar that is gradually broken down by the body.
There are many available sclerosing agents, which—based on the mechanism causing endothelial damage—are divided into three groups:
- detergents,
- hyperosmotic agents,
- corrosive agents.
The most commonly used sclerosing agent in our practice is polidocanol (hydroxy-polyethoxy-dodecane), known as Aethoxysklerol or Sclerovein, used in liquid or foam form.
CONTRAINDICATIONS
Before starting sclerotherapy treatment, all possible contraindications must be excluded.
Absolute contraindications:
- allergy to the sclerosing agent,
- deep vein thrombosis and acute thrombophlebitis,
- acute febrile illnesses,
- bedridden and immobile patients,
- severe arterial circulation disorders,
- decompensated cardiac, hepatic, or renal disease.
Relative contraindications:
- pregnancy,
- patients taking oral contraceptives,
- diabetes,
- advanced age.
WHAT TO EXPECT AFTER SCLEROTHERAPY
-
After sclerotherapy, the treated vein becomes firm to the touch, more prominent, and somewhat painful. Over time, the hardening will gradually thin and become less painful. This process may take several months. Eventually, the vein is completely broken down and is no longer visible through the skin.
-
Occasionally, skin discoloration (brown staining) may occur. Brown stains are caused by leakage of blood through the wall of the treated vein. This may happen at the injection site or along the entire length of the vein. Sometimes, the vein may rupture during needle insertion and the sclerosant may leak into the surrounding tissue. All of this may result in a brown skin mark, which is rarely permanent and usually fades over time. It is typically small and no more bothersome than the treated vein itself. However, patients should be aware of this side effect, which occurs in about 10% of cases.
-
Very rarely, small skin ulcers may occur after injection. In rare cases, the injection is sufficiently irritating to cause a minor skin ulcer. One such case has been reported per 1,900 injections. The ulcer size was smaller than the smallest coin and healed with a small scar.
-
After the injection, you will need to wear elastic bandages or compression stockings.
After treatment, the treated vein area will be covered with gauze padding or a specially shaped polyurethane foam. Over this, an elastic bandage or compression stocking (sometimes below the knee, sometimes up to the groin) will be applied. The bandaged limb must be kept in place for one day and overnight without interruption. During this time, you will not be able to shower or bathe. After one day, you will wear compression stockings or bandages for a variable period (2–3 weeks) during the day and may shower or bathe normally. Compression stockings or bandages should be worn during the day as long as there is pain.
If polyurethane foam is used, it should be removed before sleeping. In case of pain or itching, it should be removed earlier.
COMPLICATIONS
All preparations, except glycerol, may cause allergic reactions. All agents may lead to hyperpigmentation or skin necrosis. Superficial vein thrombosis or periphlebitis may also occur. Deep vein thrombosis is extremely rare.