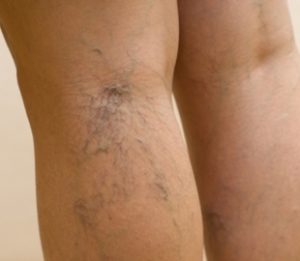
Varicose veins of the lower extremities (varices) are the result of the dilation of subcutaneous veins. Varicose veins are not only an aesthetic problem; they also cause numerous health issues and significantly reduce the quality of life.
The most common symptoms of problems with varicose veins are a feeling of heavy, tired, and tense legs, nocturnal cramps in the calves, brownish discoloration of the skin on the lower leg, itchy and burning swellings (especially around the ankles). In some people, inflammation of the superficial veins and painful ulcers (ulcus) on the lower leg may also occur. The cause of all these problems is the weakness of the connective tissue in the veins.
In healthy individuals, venous valves in the superficial and deep veins ensure the flow of venous blood toward the heart. In the case of varicose veins, the valves in the dilated vein can no longer perform this function. Blood then flows backward and returns toward the lower leg. Due to this reverse flow, blood pools in the lower leg, resulting in swelling and a feeling of tightness.
 1. HOW COMMON ARE VARICOSE VEINS?
1. HOW COMMON ARE VARICOSE VEINS?
This is a very common condition. It is estimated that 80% of the population experiences minor or major problems due to impaired venous circulation in the lower extremities, while 4% to 15% of the population has varicose veins. Approximately 1% of the population has a lower leg ulcer.
2. WHO IS MORE LIKELY TO DEVELOP VARICOSE VEINS?
-
Women are more frequently affected. Pregnancy and hormonal status play a significant role in the development of varicose veins. Both factors promote the formation of varicose veins and worsen the condition once they are already present.
-
Heredity: It is well known that varicose veins run in families. What is inherited is the weakness of the connective tissue in the vein walls and venous valves.
-
Prolonged sitting or standing: This causes the accumulation of venous blood in the veins of the lower extremities and consequently increases pressure in these veins. For this reason, varicose veins are associated with certain professions that require long periods of standing or sitting.
-
Age: The condition is also linked to aging, as connective tissue becomes weaker in older people and lifestyle tends to become more sedentary.
-
Diet can worsen venous disease in two ways: obesity caused by overeating promotes the development of varicose veins, while a diet low in fiber can lead to constipation, which also causes venous stasis.
3. WHY DO VARICOSE VEINS DEVELOP?
- Primary varicose veins occur without any obvious external cause and mainly appear in a familial pattern.
- Secondary varicose veins develop due to damage to the deep venous system. These may result from developmental abnormalities of the deep veins (such varices appear at a young age). Damage to the deep venous system leads to overload of the superficial veins, which then dilate.
4. WHAT INFLUENCES THE DEVELOPMENT OF VARICOSE VEINS?
Varicose veins are mostly an inherited condition, but there are factors that can cause earlier onset or more severe symptoms. These factors include:
-
Prolonged standing definitely contributes to the earlier development of varicose veins and more severe problems. When standing, blood accumulates in the veins of the lower extremities, and since the calf muscles do not contract as they do during walking, blood is not effectively pumped back toward the heart. Professions with a higher incidence of varicose veins include sales assistants, hairdressers, teachers, and similar occupations. People who sit for long periods also experience more problems, especially if they sit with crossed legs, which is particularly unfavorable for venous return.
-
Obesity affects the development of varicose veins for two reasons. Increased abdominal pressure makes it harder for blood to return to the heart. Obese people also move less, which weakens the action of the calf muscles that normally help pump blood upward.
-
Wearing tight clothing that compresses the groin area can impair venous flow from the lower extremities to the heart.
-
Exposure to direct sunlight and heat on the area of varicose veins causes additional increase in superficial venous flow and further dilation of the veins. This worsens the condition. Therefore, during the summer months, we recommend protecting the legs with light, breathable clothing. On the beach, the lower extremities should be protected from the sun by staying in the shade.
5. VARICOSE VEINS OR VARICOSE VEIN SYNDROME? WHAT IS THE DIFFERENCE?
-
Varicose veins are simply dilated veins that cause only aesthetic concerns without other symptoms.
-
Varicose veins with varicose vein syndrome: In addition to dilated veins, other problems are present, such as a feeling of fatigue, tension, and swelling of the lower extremities. These signs already indicate worsening of the condition and possible damage to the most sensitive tissues of the lower leg.
6. WHAT COMPLICATIONS CAN VARICOSE VEINS CAUSE?
A. Venous inflammation (phlebitis)
- Superficial veins → superficial phlebitis
- Deep veins → deep vein thrombosis
Deep vein thrombosis is a condition in which a blood clot forms in the deep veins. If not properly treated, it can lead to very serious complications. A clot in the deep veins damages the valves, which usually results in post-phlebitic syndrome. If the clot breaks off from the vein wall and travels through the bloodstream to the heart and then to the lungs, it can cause life-threatening pulmonary embolism.
B. Lower leg ulcer
This is the complication that affects the patient the most and requires long-term treatment. It is usually the result of delayed or inadequate treatment of venous disease. Today, lower leg ulcers can be successfully treated and prevented.
C. Skin changes
Skin discoloration
It first appears as small, coin-sized, reddish-brown spots on the back of the foot or around the ankle. Initially, these spots appear only after prolonged standing or rest and then disappear. Over time, the changes become permanent and spread. In advanced stages, the entire inner side of the lower leg—from the inner ankle to just below the knee—becomes reddish-brown to bluish in color.
Swelling of the lower leg
This occurs after a varying duration of venous disease. With superficial varicose veins, it is initially not very pronounced and appears after prolonged standing or an upright body position. It is therefore worse in the evening and usually disappears overnight when lying down. Swelling of the lower leg can occur in many other conditions, so only a medical examination can determine the true cause.
Skin inflammation (hypostatic dermatitis)
People usually describe the skin changes as eczema caused by inflammation. The inflammation can be dry, manifesting as redness, warmth, burning, and stinging in the affected area. Sometimes the inflammation becomes “weeping,” with clear reddish fluid oozing from the skin. Inflammatory skin changes are a sign of impaired skin circulation. Skin inflammation or eczema is the first warning sign of an impending lower leg ulcer.
7.  WHAT ARE THE TREATMENT OPTIONS FOR VARICOSE VEINS?
WHAT ARE THE TREATMENT OPTIONS FOR VARICOSE VEINS?
There are various ways to relieve symptoms and treat varicose veins. The most suitable method depends on the size, shape, and anatomy of the varicose veins, as well as your general health and personal preference.
Available options include:
- Conservative treatment with external compression of the veins using elastic bandages or medical compression stockings.
- Elimination of reverse flow (reflux) by chemical closure (sclerotherapy) of superficial veins through the injection of specific chemical agents, followed by wearing elastic bandages.
- Elimination of reflux using mechanochemical endovenous closure and removal (ablation) of damaged varicose veins with the ClariVein® system (so-called MOCA – mechanochemical endovenous ablation).
- Elimination of reflux by thermal closure and removal of varicose trunk veins – laser or radiofrequency ablation.
- Surgical procedure involving ligation and removal of varicose veins.
All procedures at our facility are performed under local anesthesia. Due to the minimally invasive nature and excellent results, we most often recommend laser treatment of varicose veins.
8. WHEN IS SURGICAL TREATMENT NECESSARY?
There are several reasons to consider surgical treatment:
- Impact on lifestyle If your job or leisure activities involve physical exertion and pain or the need to protect your legs from injury is limiting you.
- Pain Does the pain from varicose veins interfere with your work? If the varicose vein is only below the knee and there are no other problems, sclerotherapy may be sufficient.
- Appearance Are you concerned about the cosmetic appearance of your varicose veins? This is especially important for women who are in personal contact with clients at work or appear in public life.
- Skin problems If skin inflammation (eczema), darker skin discoloration, burning pain, or stinging is present, this indicates impaired skin circulation and advanced disease. Eczema can be the first sign of an impending lower leg ulcer.
- Lower leg ulcer Do you have an ulcer (wound, ulcus) on your lower leg? A venous ulcer usually appears on the skin around the inner ankle. Such an ulcer is very concerning because it heals with great difficulty, can bleed when injured, or become infected, requiring medication. The ulcer needs to be dressed daily, treated with healing ointments, and bandaged. This can take months or even years. Sometimes skin grafting from another part of the body is necessary. Ulcers are more common in older people, whose skin is less elastic—especially those who have had deep vein thrombosis in the past. Once a lower leg ulcer develops, it can take many months to heal (if it heals at all).
- Phlebitis (venous inflammation) Do you have a small area on the thigh or lower leg that feels hard, tender, and painful, with warm and reddened skin along the vein? This is a special type of superficial vein inflammation (phlebitis) associated with clot (thrombus) formation in the vein. The clot forms due to slow blood flow in the dilated and elongated vein (varicose vein). This condition is called thrombophlebitis. Much more rarely, a clot forms in a deep vein, in which case there is a possibility (fortunately rare) that the clot detaches and travels through the bloodstream to the lungs. Blood clots (emboli) in the lungs are a serious complication that can cause breathing difficulties or even sudden death. Treatment is necessary to prevent this. However, deep vein thrombosis occurs much more often after prolonged bed rest following major surgery than as a result of varicose veins. It is actually a very rare complication of varicose veins.
Clinic opening hours are by appointment only. To schedule an appointment, please use our contact form.
 1. HOW COMMON ARE VARICOSE VEINS?
1. HOW COMMON ARE VARICOSE VEINS?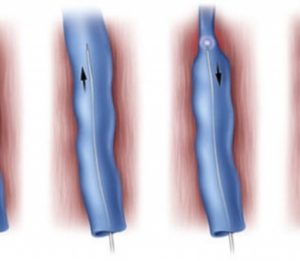 WHAT ARE THE TREATMENT OPTIONS FOR VARICOSE VEINS?
WHAT ARE THE TREATMENT OPTIONS FOR VARICOSE VEINS?